- Federal Cuts to Health Care
- Regulatory Relief
- State Budget and Health Care Financing
- Strong Partnerships Protect Patient Care
- Hospital Financial Challenges
- Optimizing Medicaid
- Rural Health
- Additional Issues
- Medical Debt
- 340B
- End-of-Life Options Act Materials
- Hospital Community Benefit
- Maternal Health
- Facility Fees
- Hospitals 101
- Hospital Discounted Care
- Hospital Rate-Setting
- Hospital Workforce
- How Hospitals Get Paid
- Improve Insurance Processes
- Medicaid Enrollment
- Medicaid RAC Audits
- Responsibly Modernizing Medical Liability Caps
- Save Our Safety Net
Health Insurance Issues
What You Need to Know:
The role of an insurance company is to pay claims for covered services provided to their members—full stop. Yet insurers have inserted themselves into clinical decision-making, and the regulatory environment allows them to override or delay care contrary to a patient’s provider. They are additionally allowed to deny coverage if a patient fails to pay premiums.
At the same time, insurance premiums, deductibles, and out-of-pocket costs continue to rise while coverage becomes more restrictive, leaving many patients underinsured. However, hospitals are legally required to provide care regardless of a patient’s ability to pay. While insurers set co-pays and deductibles, hospitals and providers are left responsible for collecting those payments.
Colorado Hospital Perspective:
A 2026 survey of CHA member hospitals and health systems revealed troubling results.
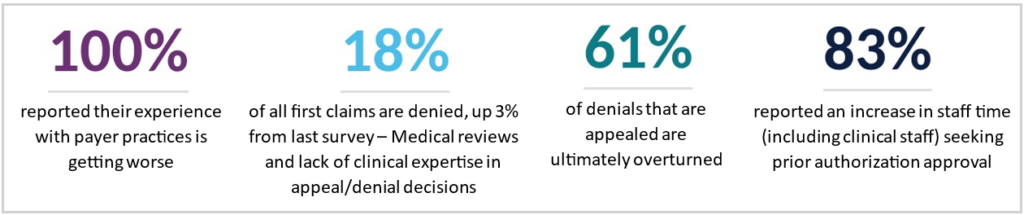
Due to recent changes by insurance companies, hospitals invest significant resources to manage health insurer requirements, diverting staff and time away from patient care. For examples:
- Colorado hospitals report findings similar to a national study by the American Hospital Association (AHA), which found that 95 percent of hospital report increases in staff time seeking prior authorization approval.
- Additional requirements add unnecessary cost to the system. In the same AHA survey, 84 percent of hospitals said the cost of complying with insurer policies is increasing.
- Carriers are not paying when services are provided to patients. Fifteen percent of all first claims are denied, and 57 percent of initial claims denials that are appeals are ultimately overturned.
Taking Action:
In 2024, CHA joined a coalition of other health care providers to create and pass legislation to fix some of the many prior authorization challenges used by insurance companies. The Health Can’t Wait Colorado coalition supported House Bill 24-1149, which will require that insurance companies eliminate or modify onerous prior authorization requirements.